Thanks to activists who have sounded alarms about campus sexual assault and workplace harassment, conversations about gender-based violence are at an all-time high. We’ve seen example after example of bad behaviour from abusers and harassers come to light, and we’re having nuanced conversations about what it means to create a “culture of consent.” But one aspect of gender-based violence that often gets overlooked in these conversations is reproductive coercion – and it’s a form of gender-based violence that is shockingly common in Canada.
Reproductive coercion occurs any time someone pressures another person about their reproductive decision-making, or takes steps that make it harder for that person to freely exercise their reproductive choice(s). It covers a range of behaviours: “stealthing” (a form of sexual assault where someone removes a condom during sex without their partner’s knowledge or consent), destroying or hiding birth control pills, breaking a promise to pull out during sex, poking holes in a condom, lying about having had a vasectomy or tubal ligation, pushing a partner to have sex during certain times in their reproductive cycle, or pressuring someone into a pregnancy or an abortion they don’t want are all examples of reproductive coercion.
Reproductive coercion has only recently been recognized as a form of gender-based violence. A 2010 article in the journal Contraception defined the concept and found, unsurprisingly, that women who faced intimate-partner violence and reproductive coercion were twice as likely to experience an unintended pregnancy.
Since that time, increased awareness of the problem has led to studies showing just how common reproductive coercion is. In a 2011 survey by the US-based National Domestic Violence Hotline, 25% of participants reported experiencing reproductive coercion. A 2017 study published in BMJ Sexual & Reproductive Health was more severe, finding that as many as one in four women accessing sexual and reproductive health care services reported not being able to freely make reproductive choices.
The consequences of reproductive coercion are dire. Victims of reproductive coercion are less able to protect themselves against sexually-transmitted infections, they are less able to plan for when or if they want to have children, and they are less able to have safe and enjoyable sex. We also know that abusers frequently use pregnancy and children as another tool to control their partners, making it harder for them to leave.
Reproductive coercion doesn’t just happen between individuals – it can happen as an institutional practice. For example, Indigenous women in Canada were being forcibly or coercively sterilized as recently as 2017. And accessing reproductive health care only just became a reality for Prince Edward Islanders – between the early 1980s and 2016, it was the only Canadian province that did not perform surgical abortions, instead forcing people to go to Nova Scotia to access the procedure.
Unfortunately, for victims of reproductive coercion, control exercised over their reproductive choices is often compounded by the gendered costs of accessing contraception.
Reproductive options targeted towards men are easily accessible, low-cost, and often free. External condoms are available at every pharmacy and distributed for free in many community centres.
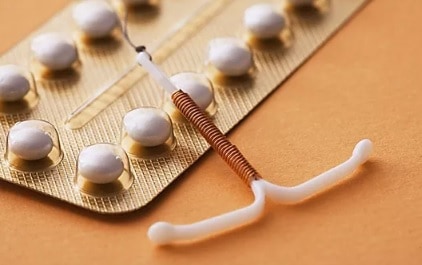
Vasectomy costs are covered by most provincial medical plans. But contraception targeting women is much more expensive and complicated – birth control pills cost about $20 per month and have to be taken consistently to be effective; intra-uterine devices (IUDs) have an up-front cost of between $75 and $380; and hormone injections cost around $180 per year. Internal condoms cost more and are harder to find.
Unless you are covered by a provincial or territorial health care program or have private insurance, those out-of-pocket costs can be daunting. For many people experiencing reproductive coercion, that abuse is one part of a spectrum of violence, which can include control over finances or private health insurance, invasions of privacy, and control over transportation – all of which make it harder to access contraception.
Tackling the causes of reproductive coercion is a long-term process – but one simple solution that could be implemented now is providing universal, no-cost coverage of prescription contraception. This is a solution currently being proposed in British Columbia by AccessBC – a grassroots, all-volunteer campaign pushing to make prescription contraception free for everyone.
Covering the costs of prescription contraception would eliminate one of the biggest barriers to contraception access, and make it much easier for people experiencing reproductive coercion to access contraception that is long-term and easier to conceal from abusive partners. It would also address the unequal burden currently faced by women, trans, and non-binary people who currently pay significantly more money to exercise their reproductive choices.
We cannot end reproductive coercion overnight, but we can make contraception easier to access. This would be an important step in recognizing that all women have the human right to make decisions around if, when, and how to create a family. All women have a right to live free from violence and discrimination, and all women have a right to health.